 OVERVIEW
OVERVIEW
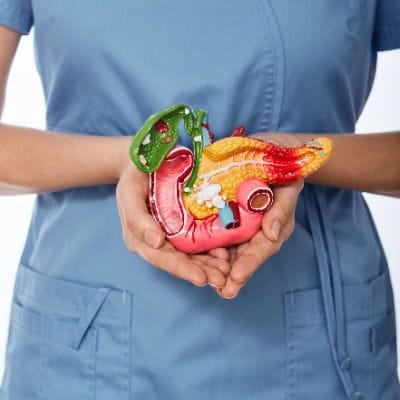
Pancreatitis is inflammation of the pancreas. Your pancreas is an organ located behind the stomach that's responsible for:
- making enzymes that help the process of digestion in the small intestine
- releasing two hormones, insulin, and glucagon, that are necessary for the regulation of blood sugar levels
Pancreatitis occurs when the pancreas produces digestive enzymes before they can be released. As a result, your pancreatic cells get affected and destroyed. This signals your immune system to attack, leading to inflammation and more cellular destruction.
What is Chronic Pancreatitis?
The first stage of pancreatitis is acute pancreatitis, which results in symptoms such as abdominal pain, nausea, and vomiting. This stage of pancreatitis is reversible and often mild for 90 to 95% of all cases. However, for the remaining 5 to 10% of patients, the damaged tissue necrotizes, leading to organ failure.
Chronic pancreatitis is a progressive inflammation of the pancreas and irreversible damage to the organ. If left untreated, it can lead to the development of pancreatic cancer.
What are the Causes of Chronic Pancreatitis?
There's no single cause of pancreatitis, however, certain risk factors can make you more predisposed to developing the condition. This can include:
- Heavy alcohol use
- Smoking
- Genetics
- Cystic fibrosis
- Gallstones
- Certain medications
What are the Symptoms of Chronic Pancreatitis?
Symptoms of chronic pancreatitis include:
- Chronic pain in your abdomen
- Recurring epigastric pain that can travel to your back
- Loss of weight
- Diabetes
- Upset stomach
- Vomiting
Patients with chronic pancreatitis are likely to develop exocrine pancreatic insufficiency (EPI), leading to loose stools, muscle cramps, pain in your bones, and pale skin that bruises easily.
The reason this occurs is due to the inability of your body to absorb vitamins and minerals from the small intestine, as digestive enzymes from the pancreas are unable to be produced.
Treatment for Chronic Pancreatitis is Safe When Performed by a Board-Certified Gastroenterologist
A physical exam with a board-certified gastroenterologist is one of the steps to accurately diagnosing pancreatitis. Your doctor may also recommend:
- CT scan or MRI of the pancreas
- Blood samples to detect lipase and amylase levels
- Stool test to check fat levels
- Endoscopic ultrasound (EUS)
- Magnetic resonance cholangiopancreatography (MRCP)
- Endoscopic retrograde cholangiopancreatography (ERCP)
Treatment for chronic pancreatitis mainly focuses on pain management. It can also include:
- Pancreatic enzyme replacement therapy (PERT)
This therapy helps restore your gut's ability to digest nutrients. - Vitamin and Mineral supplements
- Insulin for patients whose pancreatitis has caused diabetes
- Surgery to treat blockages or help in pain relief
Disclaimer:
The information on this website is provided for educational and information purposes only and is not medical advice. Always consult with a licensed medical provider and follow their recommendations regardless of what you read on this website. If you think you are having a medical emergency, dial 911 or go to the nearest emergency room. Links to other third-party websites are provided for your convenience only. If you decide to access any of the third-party websites, you do so entirely at your own risk and subject to the terms of use for those websites. Neither Arnon Lambroza, M.D., P.C., nor any contributor to this website, makes any representation, express or implied, regarding the information provided on this website or any information you may access on a third-party website using a link. Use of this website does not establish a doctor-patient relationship. If you would like to request an appointment with a health care provider, please call our office at 212-517-7570.
 OVERVIEW
OVERVIEW

